

Coccygodynia (also referred to as coccydynia, coccalgia, coccygalgia, or coccygeal pain) is a painful syndrome affecting the tailbone (coccygeal) region. The word coccyx comes from the Greek word for cuckoo (kokkyx), on the basis of this structure’s resemblance to the shape of a cuckoo’s beak (see the image below).
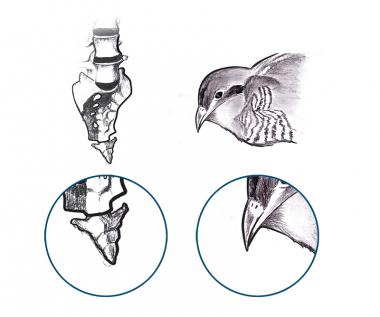 Coccyx as compared with cuckoo's beak.
Coccyx as compared with cuckoo's beak.
The pain in coccygodynia is typically triggered by or occurs while sitting on hard surfaces. The pain often varies and sometimes is aggravated by arising from the sitting position.
For most patients with coccygodynia, conservative therapy (eg, massage, injection, and ganglion impar block) appears to play a vital role in management.[1] For those with intractable pain that does not respond to conservative therapy, coccygectomy is typically effective. However, optimal specific therapy for each specific type of coccyx in coccygodynia is still a matter of debate, and no final consensus has yet been reached.
For patient education resources, see Tailbone (Coccyx) Injury and Low Back Pain.
NextCoccygodynia accounts for fewer than 1% of all back pain conditions.[2, 3, 4] It is five times more prevalent in women than in men,[5] presumably because the bone is more prominent in women than in men.[6] Although coccygodynia can occur over a wide age range, the mean age of onset is around 40 years.[5]
Several possible causes of coccygodynia have been described. The most common of these is a single axial trauma, such as occurs with a fall directly onto the coccyx or during childbirth. However, Maigne et al have suggested that only a traumatic event that occurs within 1 month of onset is significant in increasing the risk of instability and subsequent coccygodynia.[7]
Obesity is another possible cause of coccygodynia. A body mass index (BMI) greater than 27.4 in women or 29.4 in men is a risk factor for the development of both idiopathic and posttraumatic coccygodynia.[7] As high-BMI individuals attempt to sit down, the coccyx tends to jut out posteriorly as a result of inadequate sagittal pelvic rotation. This results in increased exposure to the intrapelvic pressure that occurs with sitting, ultimately causing subluxation of the coccyx.
The coccygeal configuration (see Pathophysiology) also appears to influence the cause of pain. Types II, III, and IV are more painful than type I.[8]
Coccygodynia may also occur in individuals with a normal coccyx. In such cases, the pain may derive from secondary causes, such as tumor, infection, bursitis, or posttraumatic arthritis.
The coccyx consists of three to five rudimentary vertebral units that are fused, except for the first coccygeal segment, which in turn articulates with the sacral cornu of the inferior sacral apex at S5 (see the image below). The sacrococcygeal articulation is either a symphysis or a true synovial joint.
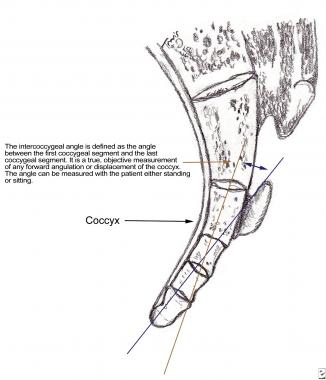 Coccyx is usually formed of 3-5 rudimentary vertebrae.
Coccyx is usually formed of 3-5 rudimentary vertebrae.
Postacchini and Massobrio[8] have classified coccygeal configurations into four types (see the image below).
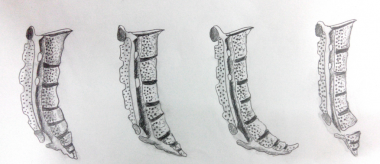 Coccygeal configuration types I, II, III, and IV (from left to right). Type I: Coccyx is curved slightly forward, with its apex directed downward and caudally. Type II: Forward curvature is more marked, and apex extends straight forward. Type III: Coccyx most sharply angulates forward. Type IV: Coccyx is subluxated at sacrococcygeal joint or at intercoccygeal joint.
Coccygeal configuration types I, II, III, and IV (from left to right). Type I: Coccyx is curved slightly forward, with its apex directed downward and caudally. Type II: Forward curvature is more marked, and apex extends straight forward. Type III: Coccyx most sharply angulates forward. Type IV: Coccyx is subluxated at sacrococcygeal joint or at intercoccygeal joint.
The majority of cases of coccygodynia occur in conjunction with either a subluxated or a hypermobile coccyx (often referred to as a culprit lesion). It has been proposed that the pathologic instability may give rise to chronic inflammatory changes and pain.[9] However, the study by Postacchini and Massobrio showed that there was no statistical difference between asymptomatic patients and those with coccygodynia in terms of the numbers of coccygeal segments or the incidence of fusions between the segments.[8]
Coccygodynia is a rare condition but can be highly unpleasant when it does occur. Patients' chief complaint is pain.
Most patients give a history of a fall or an antecedent childbirth. In 1950, Schapiro described this disorder as "television disease" because most of the patients had followed poor postural adaptation while watching television,[10] and this poor adaptation was thought to be an important predisposing factor for coccygodynia. Prolonged sitting while using a computer likewise can be a harbinger of coccygodynia.
Patients usually complain of pain that is aggravated by sitting on hard surfaces. Some patients may complain of pain during defecation and sexual intercourse or while riding a bicycle or a motorbike.
From the 1930s through the late 1960s, George Thiele published several articles relating to coccyx pain,[3] as a consequence of which coccygodynia is still sometimes referred to as Thiele syndrome. Thiele's description of the clinical features continues to hold true today. The main symptoms include pain in the lower sacrum or coccyx or in the adjacent muscles or soft tissues. The patient usually points to the coccyx as the site of pain.[1] The severity of pain depends on the amount of time spent sitting.
There is tenderness over the localized region. In fact, absence of local tenderness over the coccyx should lead the examiner to consider other diagnoses, such as lumbar disk disease or herniated disk. A rectal and pelvic examination also should be performed to check for any masses (tumors).
The differential diagnosis can be broadly divided into the the following three major categories:
The nociceptive aspect of the differential diagnosis includes conditions involving pain arising from the os coccygis,[11] such as the following:
The neuropathic aspect includes conditions in which the pain arises from the spine,[12] such as the following:
Visceral pain is the result of pain referred from the visceral structures[13] and may arise from the following:
Copyright © www.orthopaedics.win Bone Health All Rights Reserved